KNOWLEDGE HUB

If you are reading this, you have likely just logged in to your patient portal or walked out of a doctor’s office holding a piece of paper that feels more like a riddle than a report. Seeing the phrase “Variant of Uncertain Significance” (VUS) for the first time is often a confusing experience. You may feel a sudden rush of hope that you finally have an answer, quickly followed by a heavy sense of frustration when you realize that "uncertain" is the key word.
It is completely normal to feel alarmed. For many parents of children with rare or undiagnosed conditions, this result feels like being handed a map where the ink is still wet and the path is missing. This guide is designed to help you orient yourself in this complex landscape, translating the scientific jargon into plain language so you can move forward with clarity and confidence.
To understand what a VUS is, it helps to think of your child’s DNA as a massive, multi-volume instruction manual. Every human being has millions of small spelling variations in their manual. Most of these variations are what make us unique, they dictate the color of our eyes or hair, and they don’t cause health problems.
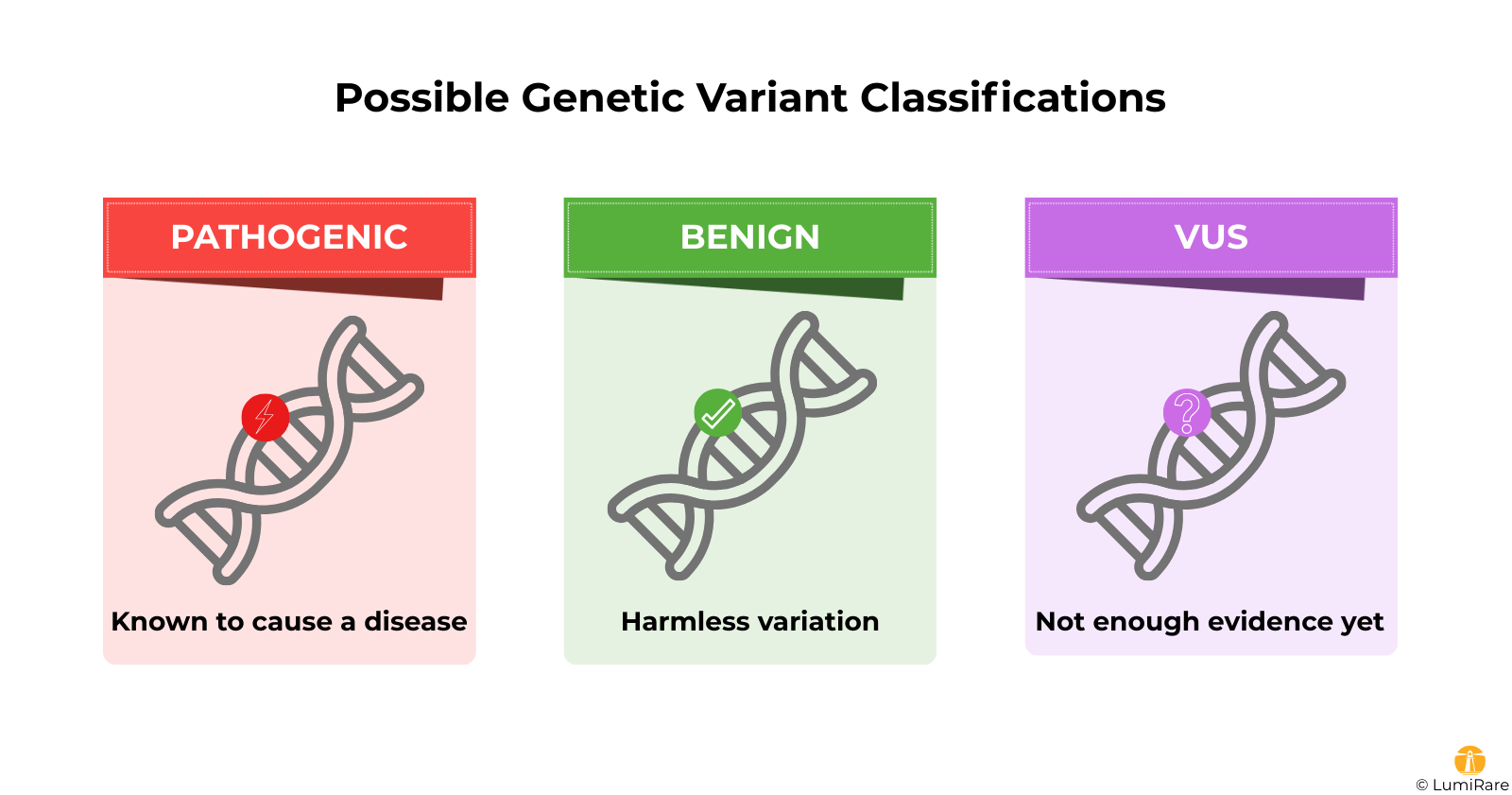
When a laboratory looks at your child’s genes, they are searching for a "typo" that might explain the symptoms you are seeing. Usually, they can put these typos into two clear boxes:
A VUS is the third box. It is a "we don’t know yet" classification. It means the lab found a change in a gene, but they don’t have enough evidence yet to say whether it is the cause of your child’s symptoms or just a harmless, rare trait. In the world of genetics, a VUS is a hypothesis that is waiting for more data to be proven right or wrong.
It can feel deeply discouraging to wait weeks or months for a test only to receive a result that feels like a "maybe". However, VUS results are actually one of the most common outcomes in modern genetic testing. This happens because every single human genome contains many variants, and many of those are extremely rare.
Science is a living, breathing process. For many rare variants, we simply haven't seen them enough times in other people to understand their impact. If your child has a genetic change that has only been documented in one or two other families worldwide, the lab cannot yet be certain about what it means. There might be a lack of functional studies, essentially lab experiments that test if that specific change stops a gene from doing its job, or there may not be enough data in large population databases to compare your child's results to "healthy" individuals.
Essentially, the technology we use to read DNA has temporarily outpaced our ability to understand everything we are reading.
This is perhaps the most important question for any parent. The short answer is: Not by itself. A VUS is not a confirmed diagnosis, and it is not definitive proof that the variant is the cause of your child’s medical challenges.
Whether a VUS becomes a "lead" or is eventually dismissed depends on the clinical context provided by your child. Doctors look at several factors to see if the VUS might be relevant. They ask if the gene is strongly linked to your child’s specific symptoms. For example, if a child has a heart condition and the VUS is in a gene known to control heart development, it raises more suspicion than a VUS in a gene related to eye color.
They also look at where the change is located on the gene level. Some parts of a gene are "critical zones", so if a change happens there, it is more likely to cause trouble. They also consider whether the variant was inherited from a healthy parent or if it is de novo (meaning it is new in the child). While these clues help build a case, a VUS remains a "maybe" until the lab has enough evidence to officially upgrade it.
One of the most helpful ways to think about a VUS is as a temporary label. Genetics is one of the fastest-moving fields in medicine, and what is "uncertain" today may be "clear" tomorrow. Reclassification happens as new information is gathered from around the world.
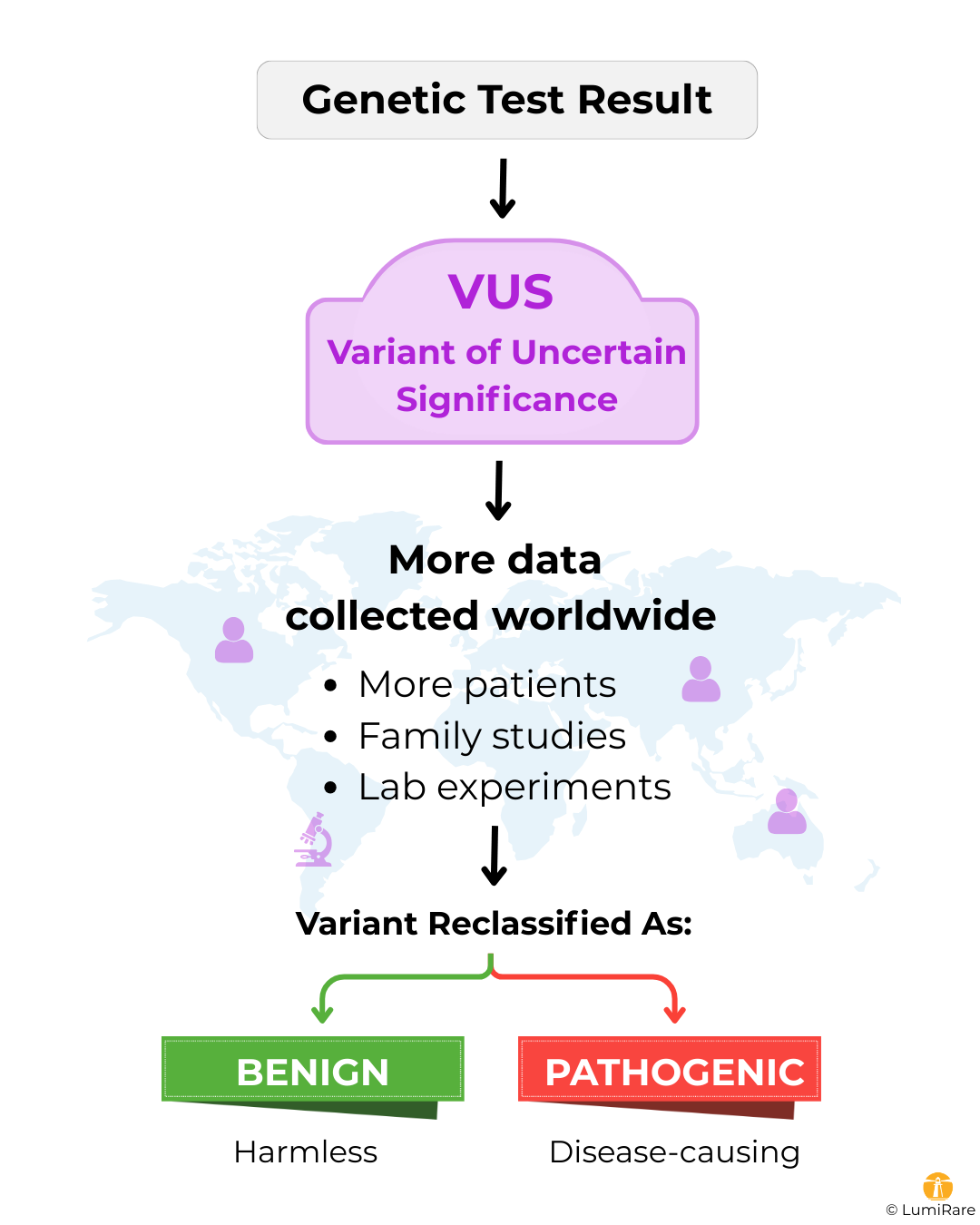
Interestingly, many VUS results are eventually reclassified as benign. As we test more and more people who don't have health issues, we often find that these "rare" variants are actually just normal parts of human diversity. On the other hand, a VUS can be upgraded to pathogenic if more families with similar symptoms are found to have the same variant, or if new lab studies prove the variant is damaging to the gene's function.
There is no set timeline for this. For some, an answer may come in a year; for others, the variant might remain uncertain for a long time if it is exceptionally rare.
Once the initial shock wears off, it is time to move into an "information gathering" phase. You don't have to be a scientist to play a vital role in this process.

First, ensure you have a copy of the full genetic report, not just the variant briefly mentioned in an e-mail. This document should contain the specific coordinates of the variant that other specialists or researchers will need to see. If possible, also request and securely store the raw genetic data files (e.g., FASTQ/BAM/VCF) in addition to the genetic report. The genome does not change over time, and these raw files can be computationally reanalyzed in the future – e.g., compared against updated medical databases as new evidence emerges.
Second, ask about parental testing. Testing you and your partner (often called "trio testing" if done at the same time as the child) is one of the fastest ways to add evidence to a VUS. If the variant is new in the child (de novo), it might increase the suspicion that it is relevant to the disease. If it was inherited from a perfectly healthy parent, it might lower the suspicion, though genetics is rarely that simple.
Third, become the expert on your child’s phenotype, which is just the medical word for their specific symptoms and traits. Variant interpretation is only as good as the clinical information the lab has. If your child develops a new symptom, or if e.g. an MRI or EEG provides new details, make sure those are shared with your genetics team. Often, a VUS is reclassified because a parent provided a more precise description of their child’s challenges, allowing the lab to see a "match" they missed before.
Fourth, you may also consider a scientist-led literature analysis such as LumiRare’s scientific report. This is not a medical service and does not provide diagnosis or treatment recommendations; instead, we map what is known about the gene identified in your genetic test and its pathway, summarize evidence across patients, model systems, and experiments, and highlight reported modulators and potential cautions from the literature. Our goal is to give you a clear, referenced scientific basis to support more focused discussions with your clinicians and, where appropriate, help identify realistic research directions to explore. You can learn more here.
This is a high-stakes area where you need to rely closely on your clinical team. Generally speaking, a VUS should not be the sole reason for making major, life-altering medical decisions. Instead, medical care should continue to be based on your child’s actual symptoms. If your child needs physical therapy or specialized monitoring for their heart, they should receive that care because of their symptoms, regardless of whether the genetic "typo" has a clear name yet.
Questions to ask your doctor at your next appointment
It is very easy to feel overwhelmed during a genetics appointment. You might find it helpful to bring this list of questions to ensure you get the clarity you need:
A Final Thought
Receiving a VUS result is like being in the "waiting room" of science. It is an uncomfortable place to be, but you are not alone. Thousands of families are in this same position, navigating the space between a "maybe" and a "yes."
While the geneticists work on the data, remember that your child is more than a string of DNA. Their symptoms are real, their progress is real, and the care they receive today is the most important thing. A VUS is a lead that may one day provide a clear path, but until then, focus on the child in front of you rather than the uncertainty on the paper.
Now that you know what a VUS is, we invite you to read our next guide to discover the specific steps science takes to move a result from "uncertain" to "confirmed."
National Human Genome Research Institute (NHGRI). Variant of Uncertain Significance (VUS) [Internet]. Bethesda (MD): NHGRI; [accessed 2026 Mar 22]. Available from: https://www.genome.gov/genetics-glossary/Variant-of-Uncertain-Significance-VUS
Pavlick DC, Frampton GM, Ross JR. Understanding variants of unknown significance and classification of genomic alterations. The Oncologist. 2024;29(8):658-666. doi:10.1093/oncolo/oyae149.
This text was written by the LumiRare team – researchers specialising in rare diseases.
This content is for educational purposes only; it does not constitute medical advice.
Would you like to find out what science has to say about your genetic finding?
LumiRare’s researchers analyse scientific articles and highlight what may be most relevant to your situation.
FOLLOW FOR RARE DISEASE
RESEARCH UPDATES